Impulse Control Disorders (ICDs) including compulsive gambling, sexual behaviors, buying and eating are common in people with Parkinson’s who also take dopamine agonists (DAs), drugs used to treat the symptoms of Parkinson’s.
In one study, 411 people diagnosed with Parkinson’s were followed for five years. During that time, the risk of developing ICDs for those who took dopamine agonists was 52%. The risk of developing ICDs was only 12% for those who had never been exposed to them.
Because ICDs can be common in people with Parkinson’s and have a profound effect on quality of life, it’s important to become more educated about them and how they may affect the goal of living well.
What are impulse control disorders?
According to Psychiatric Times, impulse control disorders are characterized by:
- The perpetuation of repeated negative behaviors regardless of negative consequences
- Progressive lack of control over engaging in these behaviors
- Mounting tension or craving to perform these negative behaviors before acting on them
- A sense of relief or pleasure in performing these problematic behaviors
People who experience impulse control disorders may or may not plan the acts; however, the acts themselves nearly always fulfill their immediate wishes, even if they are ultimately distressing to the person and make them feel out of control.
The most common ICDs reported in people with Parkinson’s are pathological gambling, hypersexuality, compulsive shopping and compulsive eating. More than 25% of the people who have ICDs have two or more of these behavioral addictions.
What are dopamine agonists?
Dopamine agonists mimic the effect of dopamine in the brain. They stimulate dopamine receptors directly without being metabolized to another compound as is the case with levodopa. Dopamine agonists are typically the most common medication used to treat Parkinson’s, aside from carbidopa/levodopa, in the early stages of the disease. This is because when compared to levodopa, long-term use of dopamine agonists may be less likely to lead to motor complications and, if they do develop, they may be less severe, though, even this belief is being challenged now. In later stages of Parkinson’s, carbidopa/levodopa and dopamine agonists are often taken in conjunction.
One of the benefits of dopamine agonists is that they have a longer half-life—they stay active in the body longer—and can have a more immediate effect on motor symptoms, especially if the immediate release option is taken.
Some of the most common side effects of dopamine agonists are:
- nausea
- low blood pressure (neurogenic orthostatic hypotension (nOH))
- leg swelling
- drowsiness
- sudden “sleep attacks”
- hallucinations
And in the most severe cases, impulse control disorders can be a side effect of dopamine agonists, due to the receptors in the brain that dopamine agonists impact the most.
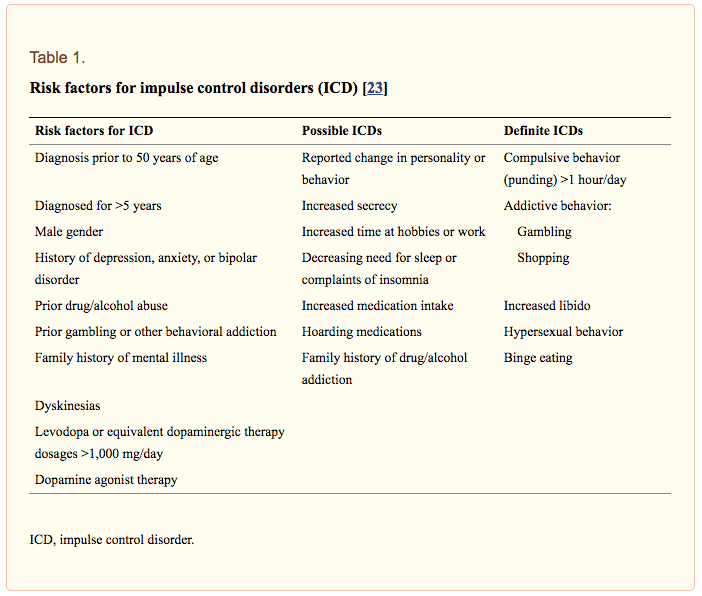
What makes someone more susceptible to developing ICDs?
Other than taking dopamine agonists, there are a variety of factors that put someone at a higher risk of developing impulse control disorders such as:
- Being male
- Age at diagnosis (YOPD)
- Longer duration of having Parkinson’s
- History of drug abuse
- Premorbid gambling
- Impulsive sensation personality traits
- Family history of psychiatric disorders
- Depression
- Overuse of dopaminergic medications due to dopamine dysregulation syndrome (DDS)
How do impulse control disorders impact people living with Parkinson’s and their care partners?
ICDs have the potential to reduce the quality of life for the person with Parkinson’s and their care partner. In some of the more severe cases, it can cause financial ruin, divorce, loss of employment and increased health risks.
ICDs can cause people to feel shameful, embarrassed and weak. They may lie to hide their addictions, act in secrecy and withdraw from their care partner or family members for fear of being found out.
In some instances, someone who has developed an ICD must also reconcile the fact that they get some level of satisfaction and pleasure from their addiction, even though it could be wreaking havoc on their lives and their most important relationships.
When we spoke to one of our community members, she shared how her husband felt shame and guilt for his sudden interest in porn and his overspending. Fortunately, he came to her and told her what was going on. They worked with his doctor, and though it’s an ongoing issue to make sure the balance of medications is best for him, the silver lining is that their relationship is strong and they’re working through it together.
We spoke to another woman whose husband had become a compulsive spender, put them in significant debt and refused to get help. It was the end of their marriage and many of the other dreams they once had. That’s an extreme example for sure, but it’s not an impossible scenario if ICDs are left unreported and untreated.
Fortunately, being knowledgeable about ICDs, risk factors and causes is an essential step for minimizing the impact on daily life.
What’s the treatment for impulse control disorders?
The most important thing to remember about impulse control disorders in people with Parkinson’s is that it’s a medical condition, not the result of personal weakness. If help is sought, it is possible to get better.
All ICD behaviors are on a continuum and where they fall on that continuum and how destructive the ICD is to a person’s life will indicate the kind of treatment needed.
For example, a male who begins taking dopamine agonists may become much more sexual than he had been in the past. He may want sex all of the time, with his wife/partner, which only seems like a big deal if he never wanted it before. However, that doesn’t necessarily mean his desire for more sex is destructive. In this case, he may need marriage counseling more than he needs medical treatment. If his sexual behaviors become pathological and destructive, that’s when a medical approach would be advised.
The first line of treatment when the behaviors are severe and destructive is to reduce the last medication that was changed in treating Parkinson’s symptoms. In the majority of cases having to do with pathological gambling, reducing or discontinuing the dopamine agonist reduced or eliminated the severity of the ICD.
People with compulsive gambling, spending or eating typically respond well to dopamine agonist reduction, whereas patients with punding benefit from reducing levodopa. The population with problems resulting from hyper-hedonistic behaviors—excessive and insatiable actions that increase pleasure—may benefit from a reduction of either dopamine agonist or levodopa.
There are those who get withdrawal symptoms when they stop taking their dopamine agonist, called dopamine agonist withdrawal syndrome (DAWS). According to Melissa J. Nirenberg from the Department of Neurology at the NYU School of Medicine, DAWS is “a severe, stereotyped cluster of physical and psychological symptoms that correlate with dopamine agonist withdrawal in a dose-dependent manner, cause clinically significant distress or social/occupational dysfunction, are refractory to levodopa and other dopaminergic medications, and cannot be accounted for by other clinical factors.”
This can be very challenging to manage. In this case, doctors will often put the person back on the dopamine agonist and then very slowly titrate them off. This can take a long time and controlling the ICD in the meantime can be a significant challenge.
The ongoing challenge for doctors is that reducing the dosage of a dopamine agonist or eliminating it all together can cause distressing symptoms for the person with Parkinson’s such as decreased motor control or an increase in non-motor symptoms.
One of the doctors we spoke to told us about a patient he worked with who was in his 80s. He couldn’t quite get the right dose for him. When he was on Mirapex, he was very engaged in his life but also addicted to pornography. When they reduced his dose, he became apathetic. His wife decided that she would rather he be engaged in his life and watching porn than be shut down and apathetic. In that instance, they put in safeguards to make sure he was being monitored.
Like many addictions, the therapies designed to curb or eliminate ICDs seek to find a replacement for the time that was previously spent engaging in the destructive behavior. Therefore, it’s critical to find something else to fill that time. Part of doing that is finding a support system, or being the support system while looking for something new to focus on during vulnerable times.
What can a care partner do if their person with Parkinson’s develops an impulse control disorder?
The best treatment for ICDs is prevention. And as a care partner, you are in a great position to advocate early and often for your person with Parkinson’s. Fortunately, doctors are much more judicious than they used to be when prescribing dopamine agonists, but it’s still important to be one step ahead of the drugs if your person with Parkinson’s and their doctors decide that a dopamine agonist is the best course of treatment.
Here are a few things you can do:
- Request a detailed counseling or information session before beginning dopamine agonist therapy (One of our community members told us how frustrated she was that her husband’s doctor never talked to them about the potential severity of dopamine agonist side effects. ICDs occur in enough cases with people who take dopamine agonists that doctors should be more forthcoming about them. As a care partner, you can advocate for that information now that you know more about them.)
- Do not be afraid to question your person with Parkinson’s about unexplained absences, secretive behavior, irritability, hiding evidence of the ICDs and monetary consequences and be sure to share this information with their doctors.
- Normalize their behaviors and remind them it’s a result of Parkinson’s and medications and not their fault. Normalizing what’s happening may make them more inclined to share their concerns with you.
- Be on the lookout for increased insomnia, missing meals, doses of medication and absences from work as these can all be potential red flags for the presence of ICDs.
- If the ICD is on a continuum that together you decide is manageable, work with your person with Parkinson’s to come up with a plan and strategies for managing the ICD. The more included the person with Parkinson’s is, the more likely they will follow through on the interventions. You want to give them as much freedom and autonomy as you can so they can still be in control of their own life, without letting go of so much that they are a danger to themselves or others.
Impulse control disorders can be highly stressful and cause a lot of pain for the person with Parkinson’s and their care partner. But it is possible to get help and treatment to reduce or eliminate their presence altogether.
What’s next?
If you or a loved one are experiencing impulse control disorders, please work closely with your movement disorder specialist to assess your unique situation and create a treatment plan that’s right for you. No two people experience ICDs in the same way so it’s critical to understand and evaluate all of your potential options. Throughout the process, be sure to make note of how you feel, how you behave and how medications or therapies are impacting you on a regular basis so your doctors and care partners can keep an up-to-date record of your experience.
We’d like to thank Dr. Mark Stacy, Dr. Anthony Lang, Dr. Daniel Weintraub and several people with Parkinson’s and their care partners for their expert guidance during the writing of this post.
For Further Study
Parkinson’s Disease – The Quintessential Neuropsychiatric Disorder
Parkinson TV – Season 2, Episode 3: Impulse Control Disorders. This video offers two rich case studies where you hear from people who have experienced ICDs and how they have learned to manage them.