During last week’s Care Partner Meetup, we had our regular cast, including the Foundation’s Executive Director, Polly Dawkins; two Foundation Ambassadors/care partners, Pat Donahoo and Gail Gitin; and me, Connie Carpenter Phinney. We were fortunate to welcome our good friend and very special guest Dr. Aaron Haug, a movement disorder specialist (MDS) who has been on several Davis Phinney Foundation webinars. Dr. Haug is a practicing neurologist at HealthONE Neurology Specialists in Denver. In his clinical practice, he focuses on Parkinson’s, tremors, and other movement disorders, with expertise in medical management and deep brain stimulation (DBS) to treat these conditions. This follow-up summarizes the key issues we discussed during our Meetup.
Getting to know Dr. Haug
We started by asking Dr. Haug why he chose to be an MDS, and he said it was because he wanted a specialty where he would develop a long-term relationship with his patients. He added he liked being in a subspecialty where he could help ease his patients’ symptoms throughout the disease progression.
How to prepare for a doctor’s appointment
I asked him how care partners can help in the doctor’s office. He discussed the need to be prepared and bring in a short list of pressing questions for him to review. Because time is always too short, he said he may only be able to properly focus on one or two items. If you need suggestions for what issues to bring up, we have several worksheets that can help. Dr. Haug also noted how important it is that we – as care partners – are there to help and how hard it is for those without care partners.
We discussed the Otter App for recording and providing a transcript of our meetings. This is a great way to keep a record and to save us from getting distracted by having to write everything down. The transcripts or recordings might also be helpful to share with others on your care team, like adult children who live out of town and want to be kept in the loop. Please do let the doctor know if you plan to record the session.
communicating with doctors
Gail also asked about using medical center portals or emails for advance communications (sending a list of questions or concerns ahead of time), which Gail noted can be helpful if some of the topics might cause embarrassment to your person with Parkinson’s. Dr. Haug encouraged this within the limits of HIPPA and to keep those succinct to respect the doctor’s ability to read the email or query in advance.
One of our listeners did note that her husband’s doctor refused to have her in the room, thus eliminating her ability to hear the treatment plan or raise concerns. Over the years, we have heard how some people with Parkinson’s prefer to attend without their care partner. This can impede our understanding of the disease, but it’s certainly a matter between you and your person with Parkinson’s. Dr. Haug welcomes care partners into his office and reminds us that he is part of the care team.
Advanced Parkinson’s
Another listener asked about the definition of advanced Parkinson’s, leading to a discussion about how Parkinson’s is staged. Dr. Haug told us that it’s not clear sometimes what the staging means because “Parkinson’s is multi-faceted and variable.” He also said one person’s worst symptom might be anxiety, but staging systems don’t address that accurately. And because the staging can be ineffective, one person could be in Stage 3 but faring better daily than someone in Stage 1. Cancer staging is prognostic and dictates care, but that’s not true for many with Parkinson’s.
Gail talked about how quickly her husband Gene declined, stating that two weeks before he passed, he’d had cataract surgery (an indication he/they expected him to live much longer). She and Dr. Haug discussed Lewy Body Dementia, which can accelerate quickly. I noted that in my person with Parkinson’s case, the disease just seemed to take over gradually, day after day. Still, I am also aware of how varied it is between individuals and even how it can vary significantly from day to day for each individual. Dr. Haug agreed and sees that those with a bad fall or pneumonia sometimes trigger a more rapid decline into more advanced stages of Parkinson’s.
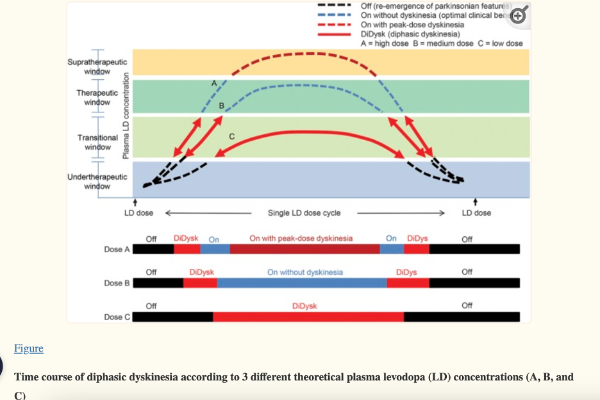
Diphasic dyskinesia
Pat relayed a recent incident with his wife, who is having an uptick in symptoms and is struggling with diphasic dyskinesia. Diphasic dyskinesia happens when the person experiences beginning-of-medication-dose dyskinesia and end-of-medication-dose dyskinesia.
I point out often how important it is to seek a second opinion or a new doctor if you are not getting the help you need from yours. Pat talked about how they had just done this two years ago because the previous doctor refused to acknowledge his wife’s diphasic dyskinesia.
Still
Next, we asked Dr. Haug if he’d seen Still, the recently released documentary about Michael J. Fox, on Apple TV and to comment on it. Specifically, I wondered if it would raise more questions than provide answers and noted I had yet to want to see it. Dr. Haug said Fox was 29 years old when he was first diagnosed and has been living with the disease now for more than three decades, and because he’s been on medication for so long, the sweet spot of when the medications work has potentially grown shorter, making his symptoms and dyskinesias much more pronounced. And in his words, it is very jarring to witness for those of us living with someone with Parkinson’s. Pat countered that it is very helpful for people curious about Parkinson’s to see Still because it helps them understand better what your person with Parkinson’s and you are dealing with. Several in the chat concurred that it was heart-warming to see Fox, especially when he was joking around with his family.
 Caloric Intake
Caloric Intake
Another question was asked about caloric intake and how to be sure your person with Parkinson’s will or can get enough calories. Gail suggested a lot of shakes while I talked about Davis’ daily smoothies. Dr. Haug suggested six small meals a day and paying particular attention to hydration to minimize the experience of dizziness (neurogenic orthostatic hypotension) upon standing. If you’d like to learn more about Parkinson’s related nutrition, click here.
What’s coming next for people with parkinson’s
We asked Dr. Haug what he saw coming down the pipeline for people with Parkinson’s, and he said subcutaneous medication could be available soon. We briefly discussed the news about a confirming test for Parkinson’s (the first of its kind) and how it will be used primarily for difficult-to-diagnose cases because it requires a spinal tap.
What has dr. haug learned from care partners
We also asked what he’s learned from care partners during his practice. He said that apathy keeps coming up, and he recognizes how hard that is to treat, much less to be around day after day. He said, “I think there’s a real dance to figuring out how to approach that, and sometimes I feel like one of the things I need to do is give care partners permission that you don’t have to keep pushing.”
Gail responded with some thoughts from her experience and said after her husband died, she wondered what she could have done differently or how she could have influenced the big picture. Gail said,
“It is a dance between the guilt that the care partner feels by not upholding their responsibility… we could have had a nicer time if I didn’t feel like I was always hounding and reminding and pushing food and doing that it becomes a full-time caregiver, not a care partner. So it’s tough. Holding hands and talking about nice things more often would have been nice.”
Holding hands more was great advice, but Gail also said, “Do yourself a favor and take it easy on yourself.”
And Dr. Haug noted how every topic we discussed had two sides, and one side was about actively pushing while the other was more passively accepting. We all noted it was an uneasy dance.
Thank you
Thanks for listening, reading, and being part of this community. Thanks especially to Dr. Haug for giving us a very valuable hour in his day.
Our next Care Partner Meetup will be on July 11, at 12 pm MDT, due to the July 4th holiday weekend. Click here to register to join us, and you can always send your questions to us via this form.
In the meantime, we’d love to know: What’s one thing you are doing right now that’s working for you that you want to share? Please shoot us an email with some thoughts at blog@dpf.org!
Additional resources
Parkinson’s Care Partner Resources
Every Victory Counts® Care Partner Manual
Parkinson’s Care Partner Digital Workbook
The Difference Between Lewy Body Dementia, Parkinson’s Disease, and Alzheimer’s Disease
SPEAK OUT! & LOUD Crowd Training
[Webinar Recording] Speech, Voice, and Parkinson’s
What is Parkinson’s Disease Dyskinesia
The Benefits of Duopa™ for People with Parkinson’s
What You Need to Know About Gastroparesis and Parkinson’s
Parkinson’s and Apathy: A Primer
5 Ways to Manage Apathy as a Parkinson’s Care Partner
[Webinar Recording] The Victory Summit Virtual Event: Care Partners
 Meet Dr. Aaron Haug, MD
Meet Dr. Aaron Haug, MD
Dr. Haug is a neurologist and movement disorder specialist at HealthONE Neurology Specialists in Colorado. He completed his pre-medical courses as well as a philosophy major with honors at Creighton University. Dr. Haug earned his medical degree at the University of Kansas. He completed neurology residency and a movement disorders fellowship at the University of Colorado, including a year as Chief Resident. In his clinical practice, he focuses on Parkinson’s, tremor, and other movement disorders, with expertise in both medical management and deep brain stimulation (DBS) for the treatment of these conditions. Outside the office, he likes to spend time with his family, play ultimate frisbee, and follow Colorado Rockies baseball.
Would you like more information
on being a Parkinson’s care partner?
You can learn much more about living well as a Parkinson’s care partner today through our Every Victory Counts® Manual for Care Partners. Click the link below to get your free manual now.
Thank you to our 2023 Peak Partner Amneal for allowing us to make the manual for care partners available and free to all.