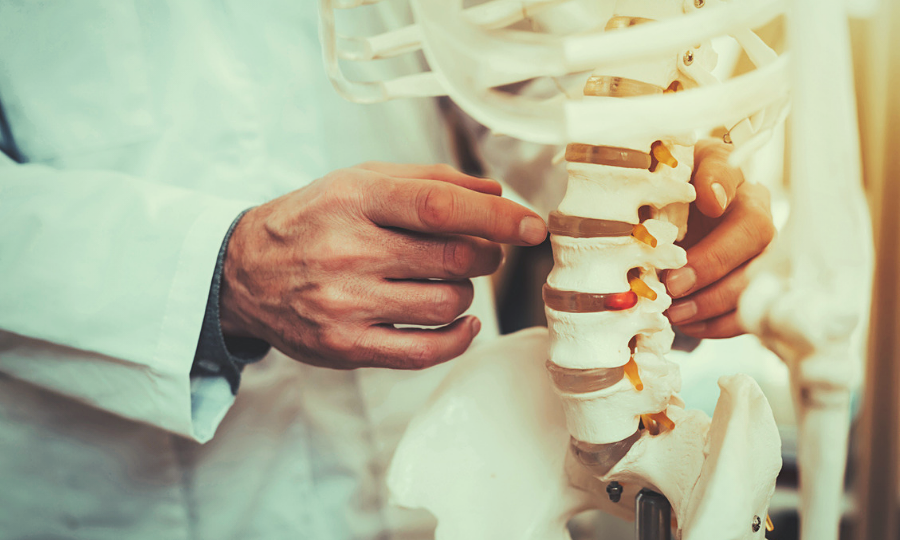
While not a direct symptom of Parkinson’s, osteoporosis, a condition in which bones become weak and brittle, is extremely common among people living with Parkinson’s. Studies have found that osteoporosis and osteopenia (the beginning of bone mass decline, which can lead to osteoporosis) affect up to 91% of women and 61% of men living with Parkinson’s. Because weak and brittle bones are easily fractured or broken, and because people with Parkinson’s are often more at risk for falls due to postural instability, it’s important to understand the causes of osteoporosis and how to prevent bone loss so you can stay healthy and mitigate your risks of getting injured during a fall.
Aging and bone health
Throughout our lives, we experience changes in bone mass. Bone is living tissue, continually being broken down, absorbed by our bodies, and renewed. When we’re young, new bone grows faster than our bodies break down old bone; this leads to strong bone mass. As we age, however, the cycle shifts, and often our bodies begin to break down old bone faster than new bone is created. This, in turn, decreases our bone mass and makes our bones more susceptible to injury.
Parkinson’s and bone health
How does Parkinson’s add to the risk of osteoporosis? A 2013 study that reviewed data from 1975-2011 about bone density and Parkinson’s reported that people with Parkinson’s have a lower bone mineral density than age-matched controls. (This 2009 study found the same thing.) The researchers found that bone loss in Parkinson’s has multiple causes (aside from the typical aging process): immobility, decreased muscle strength, low body weight, and hyperhomocysteinaemia, an independent risk factor for osteoporosis that is common in Parkinson’s because of levodopa use.
Other studies support the finding that people with Parkinson’s experience reduced bone mass due primarily to reduced mobility. Movement and weight-bearing exercise are proven ways to strengthen bones, and if you are not moving and exercising, you are not strengthening your bones.
How You Can Take Action
Although aging is irreversible, bone density loss is something you can stop. You can strengthen your bones and minimize your risk of injury (and your risk of falls themselves).
#1 – Weight-Bearing Aerobic Exercise
The first action is action itself. Weight-bearing exercise, which can help you live well with Parkinson’s in countless ways, not only helps strengthen bones but it also helps you slow mineral loss, activate bone-forming cells, build muscle, and improve balance, all of which will minimize your risk of falls and injury.
 Examples of weight-bearing exercises include walking, hiking, running, dancing, tennis, and aerobics. While other types of aerobic exercise such as cycling and swimming also offer numerous health benefits, they are not weight-bearing.
Examples of weight-bearing exercises include walking, hiking, running, dancing, tennis, and aerobics. While other types of aerobic exercise such as cycling and swimming also offer numerous health benefits, they are not weight-bearing.
If you are living with osteoporosis, talk with your health team about what exercises are safest for you to do so you can benefit from exercise while minimizing risks of fractures.
#2 – Strength or resistance training
Strength training is just as important as weight-bearing aerobic exercise, if not more, for building bone density. As your muscles move, tug, and push during resistance training repetitions, they put stress on your bones. As a result, your bones become stronger and denser.
Several times a week, complete a strength training routine that focuses on your whole body so that the bones of your hips, spine, and wrists benefit from the exercises. These bones, along with the ribs, are the places where fractures are most likely to occur, Not sure where to start with a resistance training program? A Parkinson’s physical therapist can help!
#3 – Nutrition
You likely know that calcium is essential for strong bones. Did you also know that calcium helps with many other functions such as regulating your heartbeat and nerve signals, enabling your muscles to move, helping your blood to clot, helping hormones be secreted, and more? Because your body doesn’t produce calcium, your diet must provide what you need. If it doesn’t, your body will take the calcium it needs from what is stored in your bones. This makes your bones thinner and weaker. It’s crucial that your body gets enough calcium for its many needs through the foods and drinks you consume. Dairy products such as yogurt, cheese, milk, and eggs contain calcium, as do almonds, sardines, broccoli, spinach, kale, soybeans.
 Your body needs vitamin D in order to absorb calcium. Very few food sources naturally provide vitamin D (those include tuna, sockeye salmon, rainbow trout, egg yolks, liver, and certain types of mushrooms), though many dairy products and some juices are fortified with vitamin D. Other ways to get vitamin D include supplements (be sure to talk with your doctor before starting a vitamin D supplement) and time in the sun, which, depending on where you live, the season, your skin color, and other factors, can help your body produce vitamin D. Because Parkinson’s itself can be associated with lower vitamin D levels, it is important to monitor your vitamin D levels. A blood test can determine your vitamin D level and whether supplementation is necessary.
Your body needs vitamin D in order to absorb calcium. Very few food sources naturally provide vitamin D (those include tuna, sockeye salmon, rainbow trout, egg yolks, liver, and certain types of mushrooms), though many dairy products and some juices are fortified with vitamin D. Other ways to get vitamin D include supplements (be sure to talk with your doctor before starting a vitamin D supplement) and time in the sun, which, depending on where you live, the season, your skin color, and other factors, can help your body produce vitamin D. Because Parkinson’s itself can be associated with lower vitamin D levels, it is important to monitor your vitamin D levels. A blood test can determine your vitamin D level and whether supplementation is necessary.
#4 – Other healthy lifestyle choices
Smoking and excessive alcohol consumption negatively impact your bone health. Smoking interferes with the body’s ability to absorb calcium, leading to lower bone density, and nicotine slows the production of bone-forming cells that replace bone that has broken down. Smoking can also disrupt hormone balance, especially levels of estrogen, a hormone needed to build and maintain strong bones.
Excessive alcohol consumption impacts the balance of calcium in the body, and it also interferes with vitamin D production. Like smoking, excessive alcohol consumption can also cause hormone imbalances that inhibit the production of cells that stimulate bone formation.
If smoking or excessive alcohol use are part of your lifestyle, there are many resources available to help. Talk to your doctor and other members of your care team about how to kick the habit(s).
#5 – Bone density tests
Osteoporosis often goes undetected until you experience a fracture, but you don’t need to wait for an injury to get a diagnosis. A bone density test allows your doctor to identify potential losses in bone density, determine your risk of getting broken bones, confirm a diagnosis of osteoporosis, and monitor osteoporosis treatments. Results can encourage you to begin strengthening thin bones before a fracture. Ask your doctor if a bone density test is recommended for you.
 You can’t stop aging, but you can stop the negative impacts of aging on your bones. Take action today to maintain or strengthen your bone density so you can live well with Parkinson’s, now and in the future.
You can’t stop aging, but you can stop the negative impacts of aging on your bones. Take action today to maintain or strengthen your bone density so you can live well with Parkinson’s, now and in the future.
WANT MORE PRACTICAL ARTICLES LIKE THIS?
Much more can be found in our Every Victory Counts® manual. It’s packed with up-to-date information about everything Parkinson’s, plus an expanded worksheets and resources section to help you put what you’ve learned into action. Request your free copy of the Every Victory Counts manual by clicking below.
Thank you to our 2021 Peak Partners, Adamas, Amneal, Kyowa Kirin, and Sunovion, as well as our Every Victory Counts Gold Sponsor AbbVie Grants, Silver Sponsor Lundbeck, and Bronze Sponsors Supernus and Theravance for helping us provide the Every Victory Counts manual to our community for free.