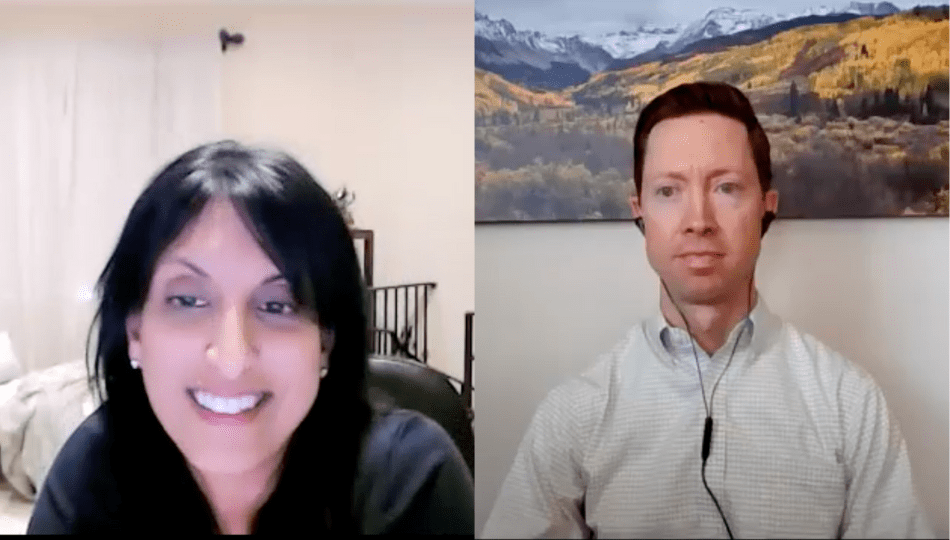
In this video, Dr. Soania Mathur and Dr. Aaron Haug discuss some basics of Parkinson’s and provide advice for people who’ve been recently diagnosed.
You can read the transcript here.
Note: This is not a flawless, word-for-word transcript, but it’s close.
You can download the audio for this webinar here: Audio Newly Diagnosed Now What Aaron Haug .
Notes
Five Things to Know about Parkinson’s When you are diagnosed
- Parkinson’s is diagnosed based on a doctor’s clinical observation of common symptoms. Today, while some tests can help with diagnosis, no test can objectively determine whether you have Parkinson’s. Some of the symptoms a doctor looks for during a clinical exam include slowness of motion that often occurs in fingers and arms, a tremor that occurs when you are at rest (called rest tremor), and stiffness or rigidity. There are also non-motor symptoms, including a loss of sense of smell, blood pressure issues, urinary urgency, difficulty regulating temperature, and constipation.
- These symptoms are not all present in everyone living with Parkinson’s, so it is important to consult with a care provider familiar with Parkinson’s if there is doubt about your diagnosis.
- The causes of Parkinson’s and the exact method of progression of symptoms are not entirely understood.
- Based on current research, only 10-15% of instances of Parkinson’s are hereditary. Research into genetic causes of Parkinson’s is ongoing.
- There is presently no cure for Parkinson’s, but there are many treatments that can effectively manage symptoms.
Frequently Asked Questions about Parkinson’s
What treatments are available?
Because research indicates that low dopamine levels is the key cause of many Parkinson’s symptoms, most treatments focus on either increasing dopamine levels or working against dopamine breakdown. There are seven main types of treatment for motor symptoms, and we have extensive information about them. The most common early treatments include:
- Levodopa, sometimes called l-dopa, is the closest thing we have to a dopamine pill
- Dopamine Agonists are synthetic dopamine that activates the same functions as dopamine
- MAO and COMT Inhibitors slow the breakdown of dopamine
When Should I start treatment?
Deciding when to begin pharmacological treatment is a personal decision, and everyone’s answer is different. The current thinking amongst many Parkinson’s specialists is that a reasonable time to start thinking about treatment is to start as soon as your quality of life begins to be affected by your symptoms. If your symptoms limit you, consider starting treatments.
What treatments should I start with?
One common option for people with mild symptoms is Rasagiline, an MAO-B inhibitor, partly because it only requires one daily dose. If your symptoms are more problematic, levodopa or dopamine agonists are worth considering. Levodopa is the gold standard, but higher doses of levodopa over an extended period can contribute to dyskinesia development. Dopamine agonists can also have significant side effects, like impulse control disorders.
Does Levodopa Become Less Effective over time?
A concern that many people have when they are newly diagnosed is whether levodopa becomes less effective the longer you take it. Current research indicates that early use of levodopa does not correspond with decreased efficacy of levodopa. The efficacy of medications is a common concern because as Parkinson’s progresses, more medications or increased amounts of levodopa are often necessary.
What Doctor should I see?
The basic answer to this question is that it is often best to see the person in your area who is most experienced in assessing and treating Parkinson’s. However, having a good rapport with your care provider is also important.
Forming a care team of multiple providers is also essential, and it is never too early to start on this. At a minimum, involve a primary care doctor and a Parkinson’s specialist, like a movement disorder specialist, if available in your area. Other care providers can be added to the team over time.
What lifestyle modifications should I make?
Eating well and remaining active are the two most accessible behaviors to help you live well with Parkinson’s.
Regarding activity, any exercise and activity is good, and more activity is often better, but there is a law of diminishing returns. You have to find the sweet spot for you at the intersection of challenge, fun, consistency, and safety. There is developing research that indicates that exercise can slow Parkinson’s progression, but what specific exercises are best is a discussion best had with a member of your care team who understands your specific circumstances, including what activities you enjoy and are safe for you to do.
Other advice
- Avoid social isolation. Find a supportive community online or in person. Social isolation can contribute to worse health outcomes.
- Be careful about misinformation. Do research with reputable organizations and consult your care team about ideas you may want to implement.
- Consider participating in clinical trials. Often, those newly diagnosed are especially valuable in clinical trials exploring new treatments, including those that aim at slowing the progression of Parkinson’s.
- While you don’t get to choose whether you are diagnosed with Parkinson’s, you can choose how you respond to your diagnosis. Choose to live well.
Additional Resources
About the SpeakerS
Dr. Soania Mathur
 Dr. Soania Mathur is a former family physician living outside of Toronto, Ontario, Canada, who resigned from her clinical practice twelve years following her diagnosis of young onset Parkinson’s at age 28. Now a dedicated speaker, writer, educator, and Parkinson’s advocate, Dr. Mathur is an active speaker in Canada and internationally at patient-directed conferences and has authored many published papers and online pieces that focus on patient education and empowerment. She serves as Co-Chair for the Patient Council of The Michael J. Fox Foundation for Parkinson’s Research, is a member of their Executive Science Advisory Board, is a member of the Board of Directors at The Davis Phinney Foundation, is part of the Editorial Board for the Journal of Parkinson’s Disease, and serves on The Brian Grant Foundation Advisory Board.
Dr. Soania Mathur is a former family physician living outside of Toronto, Ontario, Canada, who resigned from her clinical practice twelve years following her diagnosis of young onset Parkinson’s at age 28. Now a dedicated speaker, writer, educator, and Parkinson’s advocate, Dr. Mathur is an active speaker in Canada and internationally at patient-directed conferences and has authored many published papers and online pieces that focus on patient education and empowerment. She serves as Co-Chair for the Patient Council of The Michael J. Fox Foundation for Parkinson’s Research, is a member of their Executive Science Advisory Board, is a member of the Board of Directors at The Davis Phinney Foundation, is part of the Editorial Board for the Journal of Parkinson’s Disease, and serves on The Brian Grant Foundation Advisory Board.Dr. Aaron Haug
 Dr. Haug is a neurologist and movement disorder specialist at HealthONE Neurology Specialists in Colorado. He completed his pre-medical courses as well as a philosophy major with honors at Creighton University. He earned his medical degree at the University of Kansas. He completed neurology residency and a movement disorders fellowship at the University of Colorado, including a year as Chief Resident. In his clinical practice, he focuses on Parkinson’s, tremor, and other movement disorders, with expertise in both medical management and deep brain stimulation (DBS) for the treatment of these conditions. Outside the office, he likes to spend time with his family, play ultimate frisbee, and follow Colorado Rockies baseball.
Dr. Haug is a neurologist and movement disorder specialist at HealthONE Neurology Specialists in Colorado. He completed his pre-medical courses as well as a philosophy major with honors at Creighton University. He earned his medical degree at the University of Kansas. He completed neurology residency and a movement disorders fellowship at the University of Colorado, including a year as Chief Resident. In his clinical practice, he focuses on Parkinson’s, tremor, and other movement disorders, with expertise in both medical management and deep brain stimulation (DBS) for the treatment of these conditions. Outside the office, he likes to spend time with his family, play ultimate frisbee, and follow Colorado Rockies baseball.Thank You to Our 2023 Live Well Today Webinar Series Presenting Sponsors
*While the generous support of our sponsors makes our educational programs available, their donations do not influence Davis Phinney Foundation content, perspective, or speaker selection.