There are a lot of medications on the market to treat the symptoms of Parkinson’s and finding the right ones for you can take some trial and error.
In this episode with Dr. Trevor Hawkins, you will learn:
- About the most common medications that people with Parkinson’s take
- The biggest problem people with Parkinson’s face when relying on oral medications
- About current research and clinical trials that may result in better solutions in the future
- The one proven activity we know about that can slow down the progression of Parkinson’s
- About marijuana, CBD, how they work and what the research says about their efficacy
Notes
- One of the biggest issues with oral medications is that you may have a lot of ON and OFF periods
- Rytary is an extended-release combination of carbidopa-levodopa designed to maintain a steady level of relief and minimize peaks and valleys
- Duopa is a suspension form of carbidopa-levodopa that is delivered continuously by a pump through a tube into your intestine for up to 16 hours
- NeuroDerm is a continuous flow patch that is in clinical trials and may be available in 2019
- Ropinirole is an oral dopamine agonist that’s used to treat the motor symptoms of Parkinson’s
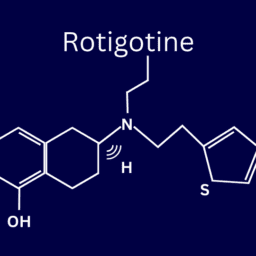
- Neupro is a dopamine agonist that is delivered via a patch
- Apomorphine is an injection to treat loss of body movement control and it’s currently in clinical trials in the US
- Current research and clinical trials are focused on developing medications that are more specific and only hit certain receptors so they produce fewer side effects
- Exercise is the one proven way to slow down the progression of Parkinson’s
- There are exciting trials being done with the cancer drug Nilotinib to test if it can modulate dopamine in people with Parkinson’s
- Using CBD oil to treat symptoms of Parkinson’s is becoming more and more common; however, the lack of oversight and inconsistency from batch to batch are big problems
- There’s a trial going on at the University of Colorado right now for a CBD pill to treat Parkinson’s tremor
- The biggest hurdle for CBD studies is that there’s no monetary support – unlike the money that big pharma companies get
- If you want to experiment with CBD oil, make sure that you tell all of your providers about it because there can be serious drug interactions and be aware that each batch you get can be very different
- There are two species of cannabis – marijuana (15-40% THC) and hemp (.3% THC)
- THC is what produces the high
- CBD oil that is derived from hemp is legal in all 50 states
- CBD oil that is derived from marijuana is not legal in every state
- There’s new research being done on CBD oil so keep an eye out for it
As with every therapy you try to treat your Parkinson’s symptoms, be sure to consult with your doctor, movement disorder specialist, neurologist and everyone on your care team. Anecdotal evidence is great; however, not everything works the same for everyone. Do your due diligence and make sure all of your experimentation is under the direct and frequent supervision of your doctors.
Concepts Mentioned in this Podcast & Further Reading
- The Neuroscience of Parkinson’s
- Living with Parkinson’s: What is OFF?
- Carbidopa/Levodopa
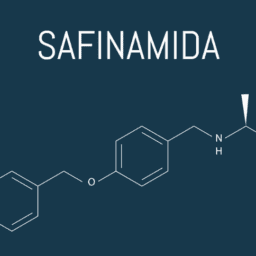
- MAO Inhibitors
- Dopamine Agonists
- What, When, Why, How & More of DBS for the Newly Diagnosed
- Exercise is Medicine for the Brain
- High-Intensity Exercise Helps Slow the Progression of Parkinson’s
- Exercise Essentials Mini Course
- Hemp Vs. Marijuana: The Difference Explained
- Is CBD Legal? Legal Status of CBD in 50 States
- Senior Citizens, Marijuana and Parkinson’s: What I’ve Learned
- My First Trip to the Marijuana Dispensary as a Person with Parkinson’s
- Can Marijuana Reduce Insomnia for People Living with Parkinson’s?
Kelsey Phinney: Last week, we learned about medications available to treat the motor symptoms of Parkinson’s and how they work in the brain. Just to recap, the three main classes of motor-specific drug therapies for Parkinson’s are carbidopa-levodopa, dopamine agonists and MAO inhibitors.
My interview with Dr. Hawkins was so awesome that I realized I had enough for two podcasts, because after he explained how the medications work, we got to talking about some newer medications available and some trials for potential medications or treatments in the future.
We talked about some research that he was just starting when we initially talked, and then he emailed me to give me an update after the summer about the research that CU Denver is doing on CBD and Parkinson’s.
Today, we’re going to delve into that.
This is the Parkinson’s Podcast™ brought to you by the Davis Phinney Foundation. I’m your host, Kelsey Phinney, and this is episode seven, part two of my interview with Dr. Trevor Hawkins.
Dr. Trevor Hawkins: Part of the reason why there probably hasn’t been an explosion of different varieties of medications working on a variety of different mechanisms, is that it’s really hard to beat levodopa. Dopamine agonists are the closest to it. A lot of the advancements we’re looking at involve fine tuning what we already know about that mechanism between the dopamine agonists and between levodopa, so we can avoid the pitfalls that come from the medication itself.
So number one, when you’re talking about Sinemet, the issue is the fluctuations that occur naturally with different concentrations. You get these peaks and valleys. Ideally, if you’re able to give a steady load, you can fine tune the amount of dopamine that the cells are receiving, so they can send out the appropriate amount of dopamine without getting too high, without getting overwhelmed, and without causing dyskinesias and not being able to produce enough to make up for the deficit. So most of the treatments are kind of trying to hone in on that.
There are some medications that are available on the market now. There’s the true long acting sinemet like Rytari, that’s the name it goes by, and it has both immediate release and the long acting, extended release sinemet.
What that allows it to do is maintain that kind of steady level that the brain is seeing for much longer periods and avoiding those peaks and valleys.
There are other pills that are coming in clinical trials that are trying to do the same kind of thing where they have to sit in your stomach and slowly diffuse out the levodopa over time to again, keep those steady concentrations. The patch is actually a very similar concept. It’s actually very similar to the insulin pumps you may have seen for patients with diabetes. You get a little pump that connects to the skin patch, a little barb that kind of digs into the medication which infuses in a steady level through the skin with the idea again, you know, to maintain that steady state level.
That one is still in clinical trial in terms of the levodopa version.
They do have one that is available for use with levodopa, which is the duopa or duodopa, which is the gastrointestinal infusion. That one is put into a feeding tube and hooked up to a pump that can infuse medication. The nice thing about that is it goes straight into your gut. So you might not have to worry about absorption issues or anything because it’s getting straight to the system and again avoid those peaks and valleys. Obviously the downside to that one is the complications that do arise from having a feeding tube and managing that.
So, the skin patch version and the pump work and potentially get the same benefit of steady infusion and hopefully, less complications. But ultimately, that’s what the clinical trials will be able to tell us.
Kelsey Phinney: To recap what Dr. Hawkins was just explaining about the levodopa therapies, the main issue with the oral medication is navigating and managing the on/off periods of when the medication is working and when it’s not, and being on that cycle throughout the day.
Dr. Hawkins explains that there are two potentially helpful newer drugs already on the market. I’m not sure how expensive these drugs are, or what that looks like.
One is Rytary, which combines fast acting and long acting carbidopa-levodopa. The other is Duopa, which is a gastrointestinal infusion. And that one’s nice because it goes straight into the gut. But it can be pretty invasive, because there’s a feeding tube involved. And then he also brings up Neuroderm, which is like an insulin pump. But with the levodopa medication in it that would again provide this continuous flow of medication, but would ideally be less invasive than the Duopa. That is in clinical trials. And from what I was reading, it might be on the market as soon as 2019. So it’ll be interesting to see how widely that gets used and if it’s helpful and effective for people navigating ON and OFF periods of Parkinson’s.
Next we get into what options are available for the second class of drugs, the dopamine agonists, and if there’s any research going into future medications for that as well.
Dr. Trevor Hawkins: The dopamine agonist has a similar concept. They actually have true extended release, once a day versions of both the Ropinirole, there’s the patch version with the Neupro patch, for example. And then in Europe since the late 1990s, they’ve had a pump that was very similar to that sinemet pump, the insulin pump, as one of the dopamine agonists called Apomorphine. Nothing to do with the actual drug morphine, it’s a dopamine agonist just like the other ones. And that one, again, is being used in Europe to do the same thing. It gets hooked up to the palm and it fuses to the skin and is a steady level throughout the day to avoid those peaks and valleys. And that’s actually currently in clinical trials here in the US. And hopefully soon, we’ll see it come available on the open market for patients. And again, the only caveat to that one is for me, like the side effects I’ve mentioned before about dopamine agonists, is sometimes that prevents patients from being able to use that but it’s very commonly used in Europe as an option for patients that would benefit from things like Deep Brain Stimulation, but aren’t able to tolerate the surgery for various reasons. And Deep Brain Stimulation is even kind of doing the exact same thing in terms of providing a constant signal in the brain to give that benefit, but give it a steady level to avoid those peaks and valleys from the medications.
Kelsey Phinney: So for dopamine agonist, we have the Nupro patch already available, and that provides that steady stream of medication throughout the day or night. And then the other thing he mentioned is the Apomorphine pump, which is available in Europe, but hasn’t been officially approved to be used in the US. Although, as he says there are clinical trials going on that might make that available soon.
And then that leads him into talking a little bit about Deep Brain Stimulation, which isn’t a drug based therapy, but it also provides continuous support for the brain to offset the symptoms of Parkinson’s. And if you’re a candidate for it, and can handle undergoing a deep brain surgery, it can be really life changing. And amazing, as has been the case with my dad.
Next I was wondering about a lot of times, especially in later stages of Parkinson’s, the OFF periods can happen quite suddenly and intensely. And I wondered what was available to try to get medication into the system quicker than with a pill. Is there anything out there? And is there anything being researched that could help with those OFF periods?
Dr. Trevor Hawkins: The interesting thing about the research is that there’s also a lot of active mechanisms to look into what you do if a patient experiences a sudden OFF, like their medications just drop out or they’re taking medication and it doesn’t really work for them, called dose failure, which tends to happen as you get into later stages of the disease. And sometimes OFF can come on and be pretty debilitating for patients.
It would be nice if we had a way to get them out of it as opposed to having to take their pill and wait a half an hour to kick in and get through their stomach and absorb it. They’ve looked at a lot of different ways – there’s one already, a dopamine agonist called Apokyn. They’re also looking at different formulations of both the dopamine agonists and Levodopa. One looks like an asthma inhaler. That way the medication gets into your lungs and goes directly into your bloodstream, and doesn’t have to sit in your gut waiting to be processed before it can get in. So the early studies, at least when you look at how quickly it kicks in, you’re talking about five to ten minutes. So for patients with that OFF that hits you out of the blue, that’s potentially very, very useful to get patients rescued out of that OFF and jumpstart the system.
Kelsey Phinney: Dr. Hawkins explains that the option already available on the market is the Apokyn injection, which is kind of like an EpiPen with dopamine agonist in it, and that delivers that medication quickly into the system. And then he also talks about the research going into creating an inhaler, similar to an asthma inhaler, that could deliver a dopamine agonist or sinemet into the system much more quickly through the lungs than through the gut. And I’m really excited to see what happens with that research. So next, Dr. Hawkins will explain some newer research going into ways to improve the medicines and their effectiveness within the brain.
Dr. Trevor Hawkins: Most of the medication trials that we have are really trying to hone in on specific receptors that it’s working on. Because levodopa kind of will work everywhere that defers dopamine and will work on all the receptors that dopamine worked on. And so sometimes that can cause the good, but with it also you get the bad if it’s hitting another receptor. It’s the same thing with dopamine agonist.
One example being those impulse control disorders, there is some evidence to suggest that if you can eliminate one type of those dopamine receptors, potentially you lower the risk of getting that side effects. So we are making medications that are more specific. It’s like if you have all these doors on the street to houses – some have red doors and white doors and black doors. If you only want it to go to the red doors, now because that’s where the good receptors are, and they give it to the white or the black, you’re getting the side effect. That’s where we can eliminate giving the message to those and only give it to the right “doors”. So that’s actually pretty fascinating to see if we can maximize the good parts of the medication and really eliminate a lot of side effects. So, I think we’re really close on having a few breakthroughs on that side of it as well.
Kelsey Phinney: I for one am very excited to see this research, I think it’s really cool. And I’m very curious to know more about how they’re able to pinpoint specific receptors or specific locations in the brain, because that would be huge and improving those negative side effects with the dopamine agonist like with a compulsive behavior. And yeah, I’m looking forward to knowing more.
Another thing that I know we’re always curious about is if there’s anything going into ways to slow down the progression of the disease. And so here’s Trevor explaining that.
Dr. Trevor Hawkins: Yeah, there is going to be a lot of active interest looking into potentially developing treatments that slow down the disease, still far and away, the most important thing now is exercise. We know it is the one thing that does slow down progression of disease. There’s definitely a lot of trials that are always ongoing, animal models, and even in the human model, and looking at medications that potentially can do it. Some kind of work in a logical manner to kind of turn down like an overactive immune system. Others have become very weird mechanisms. And some are kind of by accident, either in animal models or other humans, oh, what’s going on here, doing something to slow down progression of symptoms. Certainly we have a couple of trials over at Colorado now. One of which is looking at chemo drugs used for Hodgkin’s lymphoma. One of them showed that maybe it was slowing down the progression of disease. So right now they’re actually going to do a true placebo controlled study to see if that actually is accurate. One tricky thing in Parkinson’s, and it’s true in most diseases, is if you really believe medication is going to work for you, it will, and if you walk out the door thinking it’s not going to work for you, it won’t. Sometimes we have to be cautious about giving too much credit when it’s just the patient’s subjective improvement from the placebo effect.
Kelsey Phinney: The one proven way to prevent the progression of Parkinson’s is exercise. And we’ll actually get into more about exercise and Parkinson’s next week. But that is something to keep in mind. The other interesting research you mentioned has to do with a cancer drug that has been shown to potentially slow down the progression of Parkinson’s by pinpointing a specific protein.
But the issue with the initial study is that the patients knew that they were taking something that could slow down the progression. And so as with most drug therapy research, we have to be careful about placebo effect, which is proven that when people believe that something will work for them, even if they’re given a pill with nothing, if they think that it’s going to work, then a lot of times that’s enough to make something work.
So, they’re still doing trials that will be blind trials so that people won’t know if they’re getting the placebo or the real drug so they can actually accurately test how effective this drug could be in slowing down the progression of Parkinson’s.
We’ll close out today explaining a little bit more about CBD and what it is, why it’s being used with Parkinson’s, what kind of research is going into CBD and any precautions we should be taking about CBD. I’ll let Dr. Hawkins explain. And then I’ll come in with a follow up on some of the preliminary research findings that he emailed me about from this summer.
Dr. Trevor Hawkins: The whole marijuana, CBD, cannabinoid issue is very fascinating. Especially being in Colorado and being kind of on the front line of a lot of it. I think the big takeaway is there’s so much anecdotal evidence out there that it definitely warrants taking a deeper look at what’s actually going on.
Some of the problems with where the field is at is that there are so many different active chemical compounds within marijuana. So it’s about which are the right ones? What’s the right dose? How do you deliver it: do you have to smoke it, is it edible, does it have to be a pill? You do an ointment and with symptoms in particular, is it actually going to be helping?
So, there are still a lot of pieces to be worked out on that front. And certainly the other big problem is that there’s really no oversight. So even the individual, this is where I find a lot of issues with my patients, where they’ll tell me that they found a particular batch or strain or pill that works really, really well for them. Then they’ll get a refill and that same one that was the miracle drug is putting them in the hospital with psychosis. I think part of that is just you have to be buyer beware on a lot of that, with the current state of affairs. But I think it’s going to be an area, you know, that will hopefully take off research wise and really start honing in and hopefully the industry itself will start being a little bit more regulated – kind of similar to what we with herbal supplements and how there are self regulating groups that will still give their medication for testing to the FDA, like the Costco brands and Sam’s Club. But right now, there’s still a lot of variability.
We are going to be potentially doing a clinical trial, the second phase at the University of Colorado, hopefully sometime in the summer looking at CBD as a kind of a pill, oil suspension, and its treatment of Parkinson’s trauma. We are starting to hopefully unravel the mystery, so to speak.
We went through the phase one part of that already, which was really just looking at dose. But there are certainly a lot of hurdles when you’re talking about trying to do studies on this method. One practical point is that unlike with the medications, where you have the drug companies who are willing to fund the big trial and kind of look at if they’re working, there’s really no monetary support for looking at whether or not the CBD and marijuana products work.
That’s where some of this is being dragged out is that it’s really not as big of a push to get some of those big drug trials going. And all the federal hoops you have to jump through to make sure that that’s okay. We’ll see. We are very excited to be able to start putting together what is the right form and looking at potential CBD products and then seeing what is it going to do for us for our Parkinson patients.
The only caveat is that I tell all my patients two very important things about it:
If they are using CDB or marijuana, make sure you’re telling all your providers that you’re doing it because it is a drug that has a lot of drug to drug interactions. So it’s important to make sure that they’re dosing their other medications correctly. Just because it’s natural doesn’t mean it’s safe. Same as arsenic, it’s natural and not safe. So treat it like it’s a medication just like anything else you’re being prescribed by your doctor. That means that if you’re going to take it, you’re not immediately jumping behind the wheel of a car, you’re not down by yourself to take a bath, not putting yourself or anything in harm’s way where you wouldn’t do that with your other medications as well.
Buyer beware. Each batch is like getting a brand new medication. You don’t know 100% what it’s going to do for you; so, you’ve got to treat it as if you’ve never taken it before.
But I think it’s a very exciting time to be in Colorado. As this field is taking off, I think we’re very close to hopefully figuring out some of these things in a more scientific way about what they can potentially do for us.
Kelsey Phinney: One thing I want to reiterate is that Dr. Hawkins cautions all of us and all of you that it’s important to treat CBD like any new medication, tell your doctor if you want to try it, or if you’re already taking it. And please make sure it doesn’t interact with any of your other medicines.
Never try it before doing anything potentially dangerous like driving a car and treat every new batch you get, even from the same company, as if you’re trying it for the first time.
If you aren’t in Colorado or another state where all marijuana is legal, recreationally and medicinally, you may be wondering if CBD is even legal. I’ve done some research on CBD and we’ve come to use the terms cannabis, marijuana and hemp interchangeably in popular culture. But it turns out that those are three distinct plants. Marijuana and hemp are two species of cannabis. And the plants look different and have different chemical properties. And because of this, they have different definitions and are legal in different places.
The important thing and the primary difference chemically and medically between hemp and marijuana has to do with the two primary cannabidiol compounds found in the plants, THC and CBD. So hemp by definition contains less than 0.3% THC concentration, while marijuana can contain between 15 and 40% THC concentration. Both of these plants contain CBD as well.
THC, if you don’t know, is the psychoactive compound in cannabis. It’s what produces that high feeling when someone takes it recreationally or for medical purposes. So what does this mean? CBD oil derived from hemp is legal in all 50 states. On the other hand, CBD oil derived from marijuana is not legal in every state. So you need to research your own state’s laws, and make sure that whatever you want to take is legal and then chat with your doctor about if they think it could be beneficial and doesn’t interact with any of your current medicines.
When I reached out to Dr. Hawkins about how the research was going on CBD at CU Denver and what they’ve discovered, he got back to me in an email and explained that Dr. Leheay had completed the analysis on the phase one open label trial they did. And they were just getting started on the phase two to trial which will be the placebo controlled study.
He said that the first study showed improvement in motor scores, and the sleep and mood control portion of the Parkinson’s disease rating scale. The biggest side effects were likely in part related to the fact that they use an oil based supplement and they included diarrhea and abdominal pain. Additionally, two thirds of patients reported sleepiness and one third did have elevation in liver enzymes. He goes on to say, “My take is it most likely does have true treatment benefits, including helping with mood and sleep, and perhaps motor symptoms.” He says that it’s maybe unclear if these motor symptoms improve because of the improved sleep or mood, or if there is an independent effect on the actual motor symptoms. And he concludes his sentiment by saying “however, the adverse effects reflect the potential risks and lack of unified understanding of best dose as well as how it is prepared”.
So a couple takeaways from all of this is to hopefully give all of you a little bit more information so that you can ask your doctor questions about alternative therapies for your motor symptoms and other symptoms. And keep an eye out for new research and hopefully feel some hope that new things are in the works.
And you never know what could be truly helpful. As always, because everyone’s Parkinson’s is a little different and everyone responds differently to medications, it is so important to have an open dialogue with your doctors about anything that you even try, or take. Especially if you’re adding in a supplement like CBD, you need to be careful and check in with your doctor about it. So that’s all for this episode. Thank you so much to Dr. Hawkins for all the information. Please tune in next Wednesday for an episode about exercise. And thank you for listening.

Dr. Trevor Hawkins is an assistant professor of neurology at the University of Colorado School of Medicine Anschutz Medical Campus.
Thanks for Listening!
To share your thoughts:
- Leave a note in the comment section below.
- Ask a question by emailing us here.
- Share this show on Facebook.
To help out the show:
- Leave an honest review on iTunes. Your ratings and reviews really help, and we read each one.
- Subscribe on iTunes.











Excellent review with cogent insight regarding state of the art of current medications including a discussion of newer drug therapies. I am looking forward to learning more about the potential with use of CBD oil. I have heard that there is current research regarding regarding a medication that has the potential to arrest the progression of PD and possibly even reverse it. If such research is currently on going it would make an interesting topic for future Podcasts.
Well done! Thank you!
Thanks for listening, James. There’s so much happening in the area of medical therapies to treat Parkinson’s right now. It’s an exciting time for sure.
I have a uncle that suffers from severe Parkinson’s . He want try the CBD oil to see if it helps. Any word of encouragement.
Thanks for reading, Tommy. We always encourage people to try treatments they are interested in; however, only under the careful watch and recommendation of their doctors. Every person is different and the only way to really know what is the best path for your uncle would be for him to discuss options with this care team.
Very helpful blog,
Comment Where do I purchase CBD ? Is it very expensive ? I have very strong tremors at night on my leg and left side .It’s strong enough to push me out of bed. This happened to my sister. She was sitting at her snack bar and the tremor was so strong it took her by surprise and she fell to the hardwood floor. Her hip was dislocated.
My sister has Parkinsons too.
Hi Monica – Thank you for reading. CBD on its own (without THC) can be purchased online and in many retail locations. If you are looking for CBD and THC together, it will depend on where you live. Some states allow for recreational use of marijuana, some only for medicinal purposes. The best place to start would be your doctor, preferably your movement disorder specialist, so you can talk to them about your concerns and potential strategies to improve your tremors as well as a variety of interventions to try.
Thanks for share good information regarding New Research, Medication and CBD Oil in Parkinson’s with DR. Trevor Hawkins.
There is no mention of Parkinson’s and pain. My BFF has severe back and hip pain. Think the that neurotransmitters that result issues in movement that we are observing are just one very obvious point on a spectrum of problems caused by deficit dopamine . He has a DBS. When my BFF lies down his pain subsides. So that makes it seem more like a structural problem. However, he has had 2 different fusions in his back. We need advice regarding Locating a movement disorder specialist his 3rd one quite and moved away. Any advice would be appreciated regarding providers in the Springs, his pain, and the effectiveness of CBD oil for his pain.
Hi Sharon, Thank you for reading. I’m sorry your best friend is dealing with so much pain. When you say “the Springs”, are you referring to Colorado Springs? I think starting with a MDS is the best bet; so, I want to make sure I know where you live.
I’m in Colorado Springs with PD for almost 20 years.
Do you have any results from your trial yet? CBD is fine and if I thought it could provide help I’d try it in a heartbeat. I currently use Carbidopa Levodopa in 2 forms, er & dis, and 2 strengths. Mylan works for me. It’s getting very hard to find at any RX pharmacy. CBD could be great.
Hi Mary Lou. Thanks for reading! You can stay up-to-date on clinical trials going on in Colorado here.
How do I get in the trial at University of Colorado for CBD pill? I have Parkinson’s with dominant tremor in my right hand and arm. I want to continue teaching nursing, but my tremor is making this difficult. I live in Arizona and am willing to fly in to participate in study.
Hi Penelope – You can find detailed information about the trial here: https://clinicaltrials.gov/ct2/show/NCT03582137?recrs=a&cond=Parkinson+Disease&draw=2&rank=58
Will mention CPD to my doctor as possible treatment for my Parkinsons.
Levodopa is the most effective and most commonly used treatment for PD. This medication helps replenish the level of dopamine in the brain. Levodopa addresses many of the motor symptoms of Parkinson’s disease.
I’m 38 years old and I have Parkinson’s. I live in middle Tennessee eye not heard from the lady that works in research at Vanderbilt that CBD does help if you use it at its highest potency for six straight weeks. I would love to see if there’s any test trials for this Parkinson’s patients because I I live in middle Tennessee and I talked to a lady that works in research at Vanderbilt that CBD does help if you use it at its highest potency for six straight weeks. I would love to see if there’s any test trials for this Parkinson’s patients because I would love to be a part of the testing group because CBD can be very expensive since it is not covered through insurance.
Hi there – In order to find out about studies related to this, go to clinicaltrials.gov and then search Parkinson’s and CBD. Right now there are approximately 23 studies that are recruiting participants. Unfortunately, there are none in Tennessee at the moment, but I would check back often as there is more and more research being done on CBD.